2) Acquired causes
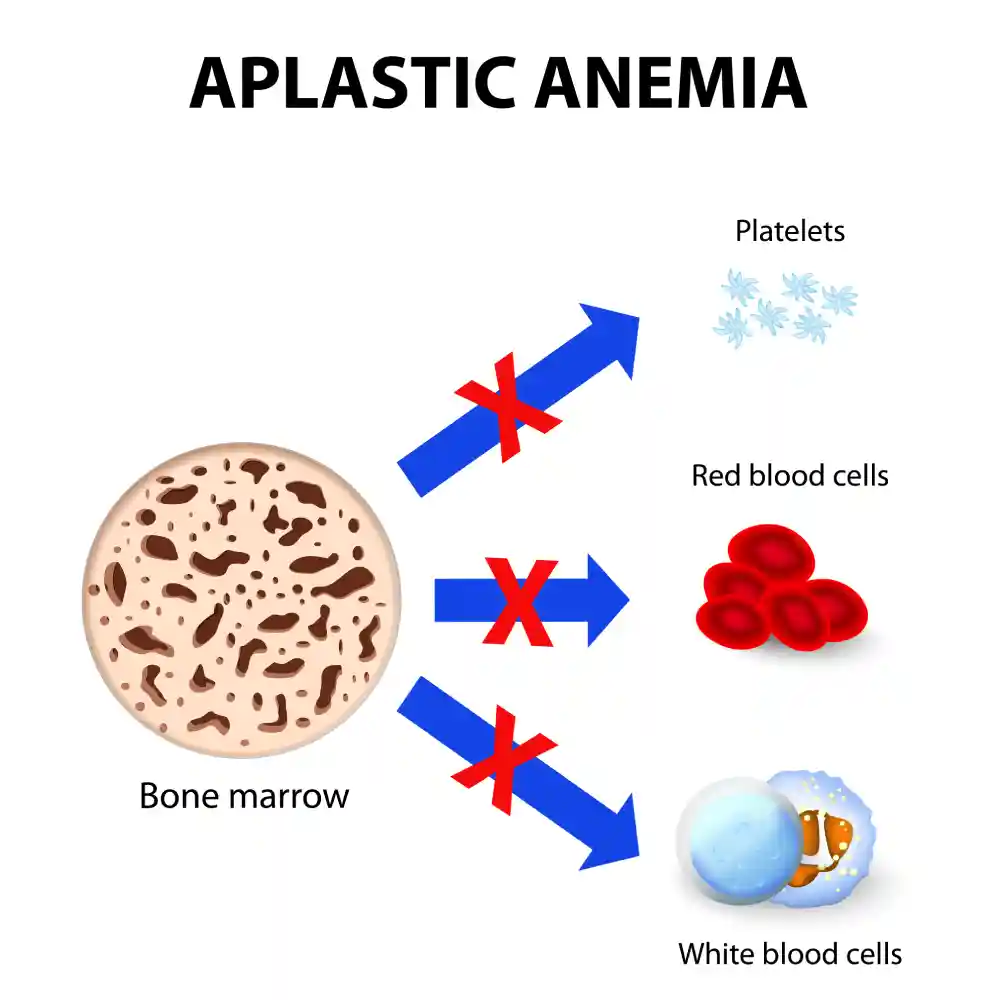
Acquired causes of aplastic anemia include:
- Infections: Infections are one of the most important causes of aplastic anemias. Some infections directly act on the bone marrow causing its suppression such as parvovirus b19 infection while others mostly damage the bone marrow indirectly via the body’s immune response. Common infections that cause aplastic anemia include: Viral hepatitis, Epstein-Barr virus, HIV and tuberculosis.
- Drugs: Some medications can suppress the bone marrow via various mechanisms. Some drugs directly damage stem cells such as chemotherapeutic agents in cancers, some act through inducing an immune reaction in the patient and others may act due to a rare genetic anomaly in some patients. The most known drugs with that side effect are: chloramphenicol, carbamazepine, phenytoin and quinine.
- Exposure to some chemicals: Some chemicals are known to have a negative effect on the bone marrow and their toxicity can result in aplastic anemia especially petrochemical products, pesticides and fertilizers.
- Radiation: Ionizing radiation exposure can have a serious effect on the bone marrow. This is usually seen in people exposed to large amounts of radiation such as cancer patients, radiologists and those working in nuclear plants.
- Cancer: Some cancers invade the bone marrow extensively enough that they encroach on the normal stem cells and decrease their capacity to produce new cells. This can be seen in acute leukemias and multiple myeloma.
- No known cause: Despite advances in modern medicine and hematology, a significant number of cases of aplastic anemia remain without a known cause.
Some anemias can result from nutritional deficiencies. This type ,however, rarely produces significant anemia unless the deficiency is severe. The main deficiencies responsible for anemia are iron deficiency anemia -which is by far the most common cause of anemia worldwide-, B12 deficiency, folate deficiency and starvation or severe protein deficiency.
Blood loss is a common cause of anemia, it can be acute or chronic. Acute loss of blood can be severe that it also produces hypovolemia and shock which puts the life of the patient in danger or it may be severe enough to cause anemia but not severe enough to cause hypovolemia. Chronic blood loss is mostly incriminated in anemia when it occurs in the gastrointestinal tract. The GIT ends in the colon which produces feces. Any source of bleeding above the colon can be completely obscured because the blood is exposed to gastric acid for long periods of time and becomes altered, causing it to be brown or tarry in color. If bleeding, however, occurs in the colon or rectum, blood will appear in stool as fresh red or dark red in color. This chronic loss of blood will produce iron deficiency which will in turn cause the anemia. Another important cause of anemia in females is the monthly menses in a female who doesn’t compensate with iron-rich food.
Causes of bleeding in the gastrointestinal tract include:
- Esophageal varices: They can be the result of end stage liver disease or bilharziasis.
- Esophageal tear: This can be the result of trauma or rupture of the esophagus (Boerhaave syndrome)
- Esophageal cancer
- Stomach ulcer: Which is a common cause of chronic blood loss.
- Stomach cancer
- Duodenal ulcer
- Duodenal cancer
- Diverticular disease: Which is an outpouching of the wall of any part of the GIT. It can get inflamed and bleeding may also occur in a minority of cases.
- Polyps: They occur in the colon or the small intestines. They are usually harmless, but can be the precursor of colon cancer.
- Inflammatory bowel disease: Both ulcerative colitis and Crohn’s disease can result in chronic loss of blood.
- Colon and rectal cancer: Colon cancer is the 2nd commonest cancer in males after lung cancer -or 3rd if we count prostate cancer-. There is a general clinical rule that any iron deficiency anemia in a male aged 40 or more is due to colon cancer until otherwise proven.
